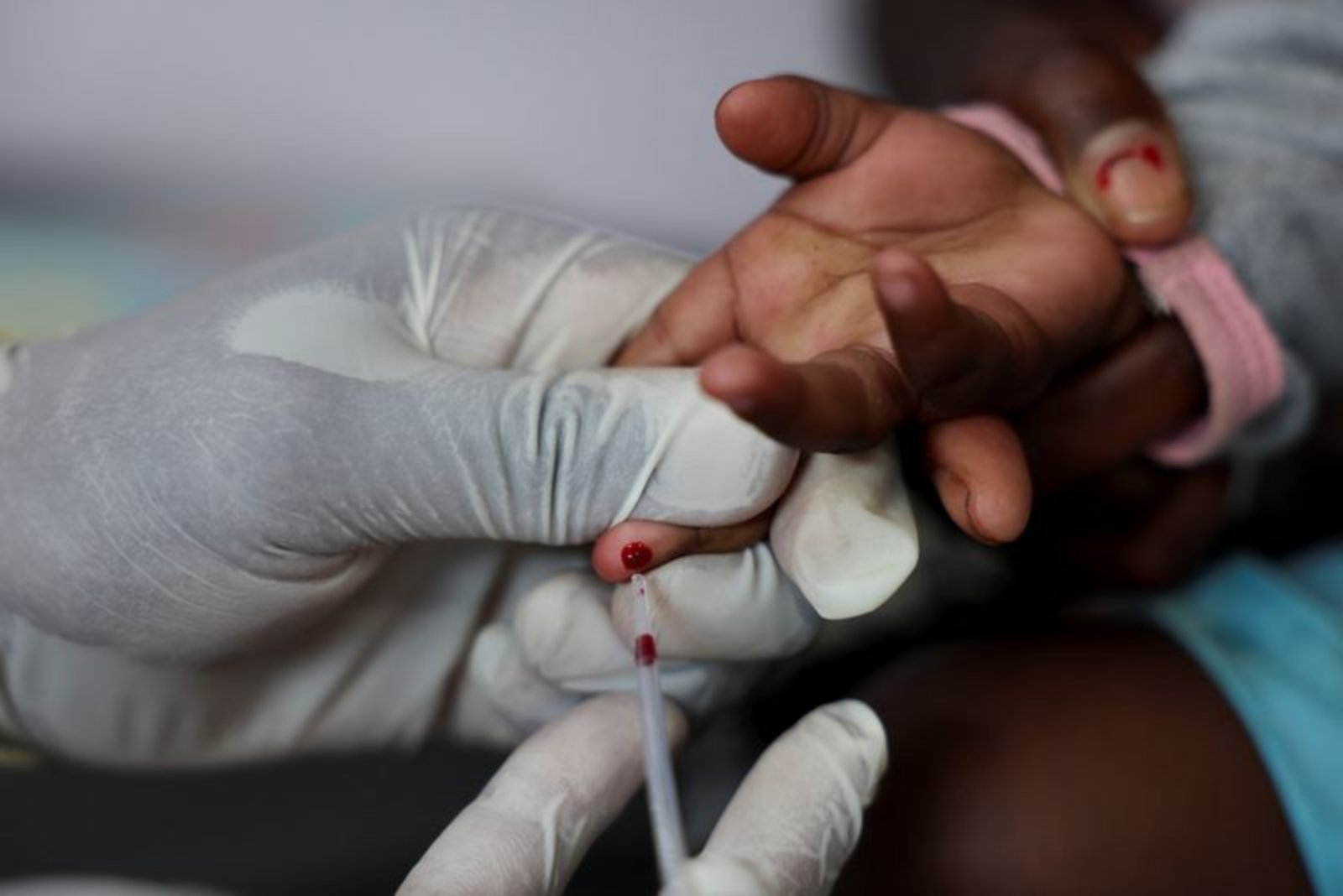
U.S. reductions in financial support have, according to a new report, dismantled HIV prevention programmes in South Africa at a moment when such services are critical to introduce a new prevention option. The report by Physicians for Human Rights, a U.S.-based non-governmental organisation, says long-standing investments in research and health delivery platforms have been abandoned, undermining efforts to connect people with prevention tools.
South Africa has the world’s largest population living with HIV, amounting to about 8 million people - roughly one in five adults. Prior to the cuts, the United States provided roughly 17% of South Africa’s HIV budget. The report notes that funding from Washington was slashed last year by President Donald Trump as part of his 'America First' foreign policy.
Those budget reductions, the report argues, have effectively wasted billions of dollars in earlier investments by allowing research infrastructure and community-facing health services to atrophy. In the near term, this weakening of programme capacity will impede the introduction and uptake of lenacapavir, a twice-yearly injectable HIV prevention drug that arrived in South Africa this month.
"We have a product that’s really powerful, but we don’t have a programme to fit it into anymore," said Emily Bass, a co-author of the report.
The report highlights that U.S. funds previously supported community-based outreach and peer education on the range of HIV prevention options. Without those outreach efforts, the report warns, potential users may be unaware that lenacapavir exists or how to access it.
Researchers found it difficult to quantify the full impact of the aid reductions in part because funding for data collection was also curtailed. Nonetheless, the report documents widespread disruption to HIV prevention activities in clinics and community settings, drawing on interviews with dozens of people involved in South Africa’s HIV response.
"We know that there are many LGBTQI communities, many sex workers, many, many young people who are not accessing services because of this," said Yvette Raphael, executive director of Advocates for the Prevention of HIV in South Africa.
The report’s findings come amid wider indicators that the cuts have affected service delivery. Last week, U.S. government figures suggested that overall HIV aid globally had been maintained despite the budget reductions; however, those data showed declines in testing and diagnoses.
South Africa’s health department and the U.S. State Department did not immediately respond to requests for comment on the report’s findings.
Context and implications
The Physicians for Human Rights report frames the aid cuts as more than a short-term budget change, portraying them as a withdrawal that has hollowed out programmes used to inform, test and treat populations at risk. By eroding outreach and data collection capacity, the report says, international funding shifts have constrained the channels through which a new prevention technology can be delivered and monitored.
Given the reported disruptions in both community and clinic settings, the immediate challenge identified by the authors is operational - rebuilding the delivery systems, outreach networks and monitoring mechanisms needed to translate the arrival of lenacapavir into broad prevention impact.